 Shin splints are an inflammatory condition of the lower leg tendons, muscles, or outer covering of the shin bone (periosteum). Exercise or athletic activities such as walking, jogging, running, or step aerobics can cause microscopic tissue damage to these areas. Normally, these small injuries heal, but when tissue damage occurs faster then tissue repair, inflammation ensues and leads to the development of shin splints. Shin splints can be separated into subcategories: anterior shin splints and posterior shin splints. Anterior shin splints would be described as pain down front and outer side of the leg, while posterior shin splints would be described as down the back and inside of the leg.
Shin splints are an inflammatory condition of the lower leg tendons, muscles, or outer covering of the shin bone (periosteum). Exercise or athletic activities such as walking, jogging, running, or step aerobics can cause microscopic tissue damage to these areas. Normally, these small injuries heal, but when tissue damage occurs faster then tissue repair, inflammation ensues and leads to the development of shin splints. Shin splints can be separated into subcategories: anterior shin splints and posterior shin splints. Anterior shin splints would be described as pain down front and outer side of the leg, while posterior shin splints would be described as down the back and inside of the leg.
 Shin splints are a very common running injury. Analysis of the biomechanics of a typical running gait may help in understanding why this injury is so common in runners. It also gives clues on how to prevent it.
Shin splints are a very common running injury. Analysis of the biomechanics of a typical running gait may help in understanding why this injury is so common in runners. It also gives clues on how to prevent it.
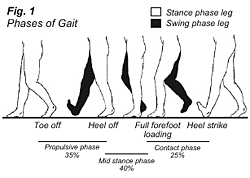
A running gait cycle consists of two phases: the swing phase and the stance phase. The swing phase begins with toe off and ends with heel strike, during which time the foot does not make contact with the ground surface. The stance phase begins with heel strike and ends with toe off, and the foot is in contact with the ground surface. In this discussion on shin splints, we will focus on the stance phase of the running gait cycle, because the stance phase is more commonly associated with this condition.
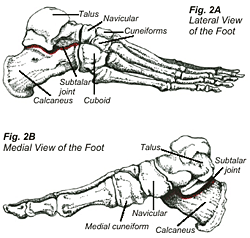
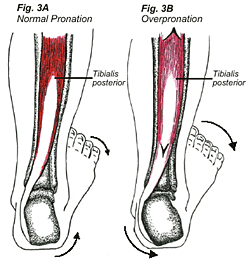 The stance phase can be divided into three phases: contact phase, mid stance phase, and propulsive phase, making up approximately 25%, 40%, and 35% of the stance phase respectively (Fig. 1). The contact phase begins at heel strike and ends at full forefoot loading (FFL), when the outer part of the foot and later the inner part of the foot make contact with the ground surface. Where the heel bone, calcaneus, and talus come together is the subtalar joint (Fig. 2A & 2B). During the contact phase, this subtalar joint pronates, which involves the heel bone tilting laterally, and the foot moving outward and upward. This movement allows the foot to be mobile, adapt to the ground surface, and absorb the shock of impact (Fig. 3A).
The stance phase can be divided into three phases: contact phase, mid stance phase, and propulsive phase, making up approximately 25%, 40%, and 35% of the stance phase respectively (Fig. 1). The contact phase begins at heel strike and ends at full forefoot loading (FFL), when the outer part of the foot and later the inner part of the foot make contact with the ground surface. Where the heel bone, calcaneus, and talus come together is the subtalar joint (Fig. 2A & 2B). During the contact phase, this subtalar joint pronates, which involves the heel bone tilting laterally, and the foot moving outward and upward. This movement allows the foot to be mobile, adapt to the ground surface, and absorb the shock of impact (Fig. 3A).
The midstance phase begins with FFL and ends when the heel begins to lift off of the ground surface. During the midstance period and into the propulsion period, the subtalar joint supinates, making the foot a rigid lever for effective toe off. This supination, which is the opposite of pronation, involves the heel tilting medially and the foot moving downward and inward.
Causes of Shin Splints
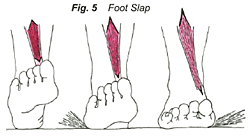
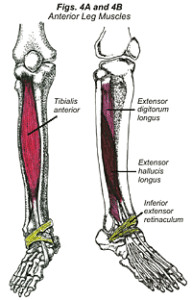 The anterior musculature of the leg — tibialis anterior, extensor digitorum longus, and the extensor hallucis longus (Fig. 4A & 4B) — decelerate the foot as it approaches the ground surface for impact before FFL (Fig. 5). Running on too many downhills and/or increasing running distances too quickly predispose a runner to developing anterior shin splints. This is because of the increased demand on the anterior leg muscles to decelerate foot slap. Driving long distances with the foot pressing on the gas pedal can also lead to fatigue of the anterior leg musculature and the development of anterior shin splints.
The anterior musculature of the leg — tibialis anterior, extensor digitorum longus, and the extensor hallucis longus (Fig. 4A & 4B) — decelerate the foot as it approaches the ground surface for impact before FFL (Fig. 5). Running on too many downhills and/or increasing running distances too quickly predispose a runner to developing anterior shin splints. This is because of the increased demand on the anterior leg muscles to decelerate foot slap. Driving long distances with the foot pressing on the gas pedal can also lead to fatigue of the anterior leg musculature and the development of anterior shin splints.
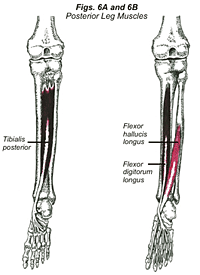
In a normal-functioning foot, pronation of the subtalar joint occurs only during the contact phase and early mid stance phase, turning the foot into a mobile lever so it can adapt to the underlying terrain. The posterior muscles of the leg that decelerate pronation of the subtalar joint are the tibialis posterior, flexor hallucis longus, and the flexor digitorum longus (Fig. 6A & 6B). Overpronation of the subtalar joint (Fig. 3B) during the contact or prolonged pronation into the midstance and propulsive phase, can lead to fatigue, microtrauma, and inflammation of the posterior leg musculature. This results in the development of posterior shin splints. Runners flat feet, when weight bearing causes the inside arch of the feet to disappear, will be prone to posterior shin splints because of the above pronation disorders. A custom made semi-rigid orthotic supporting the inside arch of the foot would help to alleviate the increased trauma on the posterior leg musculature by decreasing overpronation during the stance phase. Running on uneven surfaces will cause the uphill foot to overpronate, which is the body’s way of attempting to correct for leg length discrepancy on the un even terrain. This overpronation increases the risk of developing posterior shin splints on the uphill leg. Repetitive jumping activities can also overstrain the posterior leg musculature.
Checklist for the Prevention of Shin Splints
Change sneakers every 250-400 miles (at this point the sneaker can lose up to 40% of its shock absorption capabilities).
- Limit the number of hills on the running route.
- Avoid training on uneven surfaces.
- Slowly increase running mileage (the rate of increase will depend on your goals, activity level, and body type).
- Mix heavy intensity training with light intensity training, and include at least 1-2 days of rest from running during the week. Excessive training will cause depletion of glycogen stores in the leg musculature, leading to fatigue and eventual injury. A heart rate monitor may help runners train at appropriate intensities in their training program, helping to prevent overuse injuries.
- For runners, cross-train with swimming, biking, and the elliptical machine; this will maintain aerobic capacity and help in the prevention of shin splints.
- Add a flexibility and strength-training program for the lower leg to prevent muscular imbalances that can lead to injury. For example, tight calf muscles, including the gastrocnemius and soleus musculature, can cause weakness in the anterior leg musculature, which is responsible for decelerating foot slap, predisposing a runner to anterior shin splints.
- After finishing a run, stretch and then ice the lower extremities for 20 minutes to decrease inflammation.
Treatment of shin splints at Dr. Dubin’s office would consist of:
- Deep tissue procedures to the lower leg musculature to free up soft tissue motion
- Adjustments of the foot and ankle articulations to free up joint motion
- Ultrasound and electric muscle stimulation combotherapy to restore normal muscle tone, decrease pain, and absorb scar tissue
- Implementation of a personalized home strengthening and flexibility program
- Possibly a properly fitted semi-rigid orthotic can also be effective in the treatment of shin splints

