Plantar fasciitis is a common injury in people whose activities involve a lot of running, jumping, standing, or walking. The main symptom of plantar fasciitis is pain on the bottom inside arch of the foot. When we examine the biomechanics of a foot step, it becomes clear why this repetitive strain injury occurs, how to treat it, and how to prevent it.
 Each step can be broken down into two phases: the stance phase and the swing phase. The stance phase occurs when the foot is making contact with the ground surface. This phase can be divided into three periods: the contact period, mid stance period, and propulsive period (Fig. 1). The second phase is the swing phase, which occurs after toe off and before heel strike, when the leg is not in contact with the ground surface.
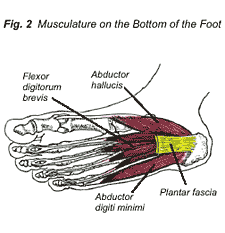
Each step can be broken down into two phases: the stance phase and the swing phase. The stance phase occurs when the foot is making contact with the ground surface. This phase can be divided into three periods: the contact period, mid stance period, and propulsive period (Fig. 1). The second phase is the swing phase, which occurs after toe off and before heel strike, when the leg is not in contact with the ground surface.
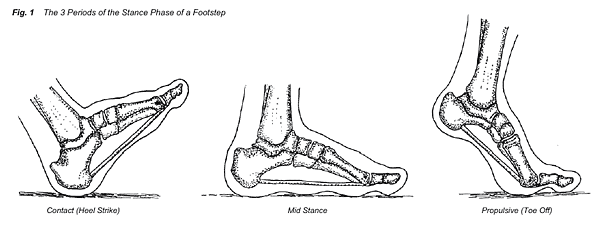
During heel strike, muscles on the front of the leg decelerate the foot and soften the impact with the ground surface. The outside of the foot initially makes contact with the ground, and as the foot adapts to the terrain, the inside of the foot then makes contact, marking the beginning of the mid stance phase. During the early mid stance phase, the muscles on the bottom of the foot are active in stabilizing the lower limb as it adapts to the ground surface. In the later stage of mid stance and the beginning of the propulsive period, when the heel lifts off the ground, the big toe is dorsiflexed (bent upwards) by the ground surface. This dorsiflexion of the big toe stretches the musculature and fascia on the bottom of the foot (Fig. 2). Fascia is a sheath of fibrous tissue that encloses muscles and muscle groups. Strain to the fascia and musculature on the bottom of the foot can be caused by excessive standing, walking, or running, and is complicated by flat feet, high arches, and improper footwear.
Case Study
Walter came to Dr. Dubin’s office with complaints of chronic pain on the bottom/instep of his right foot, which was most severe when he took his first few steps in the morning. He was frustrated because the treatments he had received for his foot over the last three years had proven ineffective. The numerous orthotic devices that were custom molded for his feet did not improve his condition. X-rays taken of his feet revealed bone spurs at the bottom of the heel of both feet, and a podiatrist convinced Walter that this was the cause of his heel pain. Dr. Dubin explained to Walter that studies have shown that these bone spurs may be coincidental findings, and pointed out that he had no pain in his left foot, where bone spurs were also present.
Walter explained that his work required a lot of standing and walking. His shoes were worn down and not well padded, and observation of Walter’s gait with his shoes and socks off revealed that he had flat feet and favored his right side. After conducting an examination of Walter’s right foot, Dr. Dubin diagnosed him with plantar fasciitis.
 Treatment of Walter’s plantar fasciitis consisted of specialized muscle work to free up soft tissue motion of the foot and surrounding musculature. Adjustments were utilized to free up joint motion in the foot and ankle, and ultrasound and electric stimulation were utilized to relax the musculature and restore normal muscle tone. Walter was advised to follow this plan: a stretching and strengthening exercise routine for the lower extremity using the Flex-Band®; rolling a golf ball under the medial arch of his foot (for ischemic compression therapy of the plantar musculature and fascia [Fig. 3]); and application of ice 20 minutes on, 1 hour off, to decrease inflammation. Dr. Dubin also recommended that he invest in a new pair of running sneakers for good shock absorption and comfort, since sneakers lose about 40% of their shock absorption capabilities after approximately 250 miles; they should be replaced every four to six months.
Treatment of Walter’s plantar fasciitis consisted of specialized muscle work to free up soft tissue motion of the foot and surrounding musculature. Adjustments were utilized to free up joint motion in the foot and ankle, and ultrasound and electric stimulation were utilized to relax the musculature and restore normal muscle tone. Walter was advised to follow this plan: a stretching and strengthening exercise routine for the lower extremity using the Flex-Band®; rolling a golf ball under the medial arch of his foot (for ischemic compression therapy of the plantar musculature and fascia [Fig. 3]); and application of ice 20 minutes on, 1 hour off, to decrease inflammation. Dr. Dubin also recommended that he invest in a new pair of running sneakers for good shock absorption and comfort, since sneakers lose about 40% of their shock absorption capabilities after approximately 250 miles; they should be replaced every four to six months.
Walter’s plantar fasciitis improved after 4 to 5 visits, and was resolved in 12 visits. Walter continues his exercise routine, and is relieved that he is finally pain-free.

