 Patellofemoral Syndrome (PFS), pain in the front of the knee, is one of the most common complaints of athletes and active people. PFS is typically caused by a repetitive strain injury or a single traumatic event. Repetitive strain injuries occur when micro-tears in the muscles, tendons and ligaments surrounding the knee joint occur faster then tissue repair, while a single event is often a fall or other athletic impact. PFS is usually characterized by a dull aching pain on the front, bottom, or top of the knee, sometimes accompanied by swelling of the knee joint. Failure to treat this injury appropriately may lead to increased pain symptoms, further damage to the structures stabilizing the knee joint, and eventually an inability of the injured knee to support body weight. This syndrome commonly occurs in athletes or the “weekend warrior” participating in sports such as basketball, football, soccer, triathlons, or track and field events. These sports involve repetitive running, jumping and sometimes kicking, placing a lot of tension on the structures supporting the knee joint.
Patellofemoral Syndrome (PFS), pain in the front of the knee, is one of the most common complaints of athletes and active people. PFS is typically caused by a repetitive strain injury or a single traumatic event. Repetitive strain injuries occur when micro-tears in the muscles, tendons and ligaments surrounding the knee joint occur faster then tissue repair, while a single event is often a fall or other athletic impact. PFS is usually characterized by a dull aching pain on the front, bottom, or top of the knee, sometimes accompanied by swelling of the knee joint. Failure to treat this injury appropriately may lead to increased pain symptoms, further damage to the structures stabilizing the knee joint, and eventually an inability of the injured knee to support body weight. This syndrome commonly occurs in athletes or the “weekend warrior” participating in sports such as basketball, football, soccer, triathlons, or track and field events. These sports involve repetitive running, jumping and sometimes kicking, placing a lot of tension on the structures supporting the knee joint.
An understanding of the anatomy and the biomechanics of the knee joint during flexion (bending) and extension (straightening) of the leg will make it easier to comprehend how to effectively treat and prevent Patellofemoral Syndrome.
Anatomy of the Knee Joint
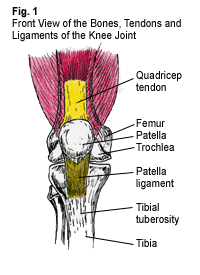
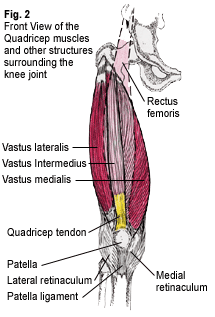 The patella, or kneecap, is a conical shaped bone lying between the femur (thigh) bone and the tibia (lower leg) bone (Fig.1). The undersurface of the patella glides over the trochlea, a groove located at the bottom and front of the femur bone. The quadricep muscle group, which plays a vital role in the stability of the knee, is located on the front of the thigh and consists of four muscles, the vastus lateralis, vastus intermedius, vastus medialis and the overlying rectus femoris (Fig. 2). The quadricep muscles share a common tendon, the quadricep tendon, which anchors these muscles onto the top of the patella. The patella ligament acts as a downward continuation of the quadricep tendon, originating from the bottom of the patella and inserting onto the tibial tuberosity, an outgrowth of bone on the front of the tibia.
The patella, or kneecap, is a conical shaped bone lying between the femur (thigh) bone and the tibia (lower leg) bone (Fig.1). The undersurface of the patella glides over the trochlea, a groove located at the bottom and front of the femur bone. The quadricep muscle group, which plays a vital role in the stability of the knee, is located on the front of the thigh and consists of four muscles, the vastus lateralis, vastus intermedius, vastus medialis and the overlying rectus femoris (Fig. 2). The quadricep muscles share a common tendon, the quadricep tendon, which anchors these muscles onto the top of the patella. The patella ligament acts as a downward continuation of the quadricep tendon, originating from the bottom of the patella and inserting onto the tibial tuberosity, an outgrowth of bone on the front of the tibia.
The two retinacula, sheath-like structures located on the front of the knee, are also important in knee stabilization. The lateral retinaculum attaches to the vastus lateralis and iliotibial band superiorly and descends to attach to the lateral aspect of the patella ligament. The medial retinaculum attaches to the lower part of the vastus medialis and descends to attach to the inside area of the patella ligament (Fig.2).
Biomechanics of the Knee Joint
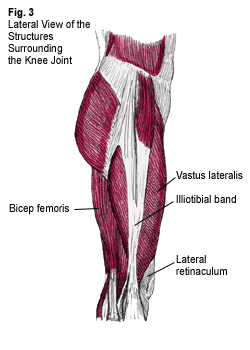
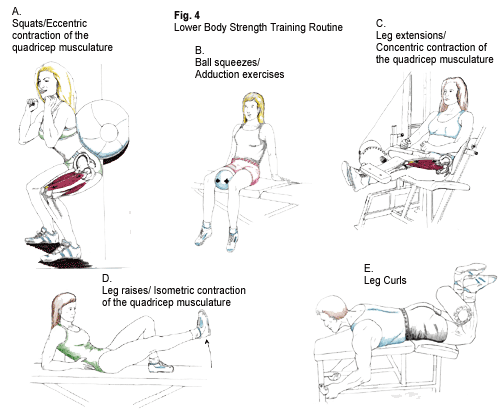
The patella acts as a pulley system by supporting the mechanical work of the quadricep musculature during leg extension and also during deceleration of leg flexion. Proper function of this pulley system depends on the ability of the patella to track properly during leg extension and flexion. Muscle tightness in the outer knee area and muscle weakness in the inner knee area may compromise this tracking, and are often a root cause of knee injury. The structures that are often tight include those on the outside of the knee, such as the lateral retinaculum, vastus lateralis and iliotibial band (Fig. 3) while structures that are often weak include those on the inside of the knee, such as the vastus medialis and adductor magnus. In this situation, the patella may track too far laterally (towards the outside of the knee). Excess lateral tracking of the patella will decrease the efficiency of this pulley system during leg flexion and leg extension, predisposing these tissues to injury. A stretching program with the Flexband© and strengthening program incorporating squats and ball squeezes (Fig. 4A & 4B) will aid in tracking the patella properly and decreasing the risk of injury.
 There are three main types of muscle contractions: concentric, eccentric, and isometric. Each of these contractions may contribute to PFS in different ways. During a concentric contraction, a muscle shortens to perform a particular motion. The patella, quadricep muscle, quadricep tendon, and patella ligament create the “extensor mechanism” of the knee. When the quadricep muscles concentrically contract, they pull on the quadricep tendon, causing tension on the patella and patella ligament, leading to extension of the leg (Figure 4C). An athlete’s ability to kick a soccer ball or football is dependent on the concentric strength of the quadricep muscles and also on the flexibility of the hamstring musculature. The hamstring muscle group acts to decelerate extension of the leg. Inadequate flexibility of the hamstring musculature will place an increased strain on the quadricep muscles during leg extension, predisposing the athlete to the development of PFS.
There are three main types of muscle contractions: concentric, eccentric, and isometric. Each of these contractions may contribute to PFS in different ways. During a concentric contraction, a muscle shortens to perform a particular motion. The patella, quadricep muscle, quadricep tendon, and patella ligament create the “extensor mechanism” of the knee. When the quadricep muscles concentrically contract, they pull on the quadricep tendon, causing tension on the patella and patella ligament, leading to extension of the leg (Figure 4C). An athlete’s ability to kick a soccer ball or football is dependent on the concentric strength of the quadricep muscles and also on the flexibility of the hamstring musculature. The hamstring muscle group acts to decelerate extension of the leg. Inadequate flexibility of the hamstring musculature will place an increased strain on the quadricep muscles during leg extension, predisposing the athlete to the development of PFS.
During an eccentric contraction, a muscle will slowly elongate to decelerate a particular motion. While doing a squat (Fig. 4A) or during heel strike and mid-stance of the running gait cycle, the quadricep muscles, tendon, and patella ligament slowly elongate to decelerate leg flexion. Excessive eccentric loads (e.g. doing a squat with weights that are too heavy, or landing from a high jump) or repetitive eccentric motions (e.g. landing from frequent jumping, as in basketball) may lead to injury of the above structures and to the development of PFS.
During an isometric contraction, the muscle generates force but neither elongates or shortens, so such movement will not lead to injury. For example, the quadricep muscles isometrically contract when conducting a straight leg raising exercise (Fig. 4D). Isometric exercises are useful in the initial stages of rehabilitation by restoring strength of the “extensor mechanism” without compromising the structure or integrity of the joint.
Checklist for the prevention of Patellofemoral Syndrome:
- Conduct a lower body strength training program (see Fig. 4A-4E). In addition to these movements, the program should include strengthening of the calf musculature, tibialis anterior, and core abdominal musculature.
- After exercise, stretch with the Flexband and ice both knees for 20 minutes.
- Cross train, rather than repeating one activity over and over. Substitute biking, cycling, and swimming for running, for example.
- Slowly increase the duration or intensity of the training program; use the 10% increase in mileage per week rule.
- Change sneakers every 250-400 miles, run on softer surfaces, and avoid hill training before a base of training is established.
Treatment of Patellofemoral Syndrome at Dr. Dubin’s office would consist of:
- Deep tissue procedures to the quadricep musculature and surrounding knee structures to free up soft tissue motion
- Mobilization of the patella and adjustments of the ankle and foot to free up joint motion
- Ultrasound and electric muscle stimulation combo-therapy to restore normal muscle tone, decrease pain, and absorb scar tissue
- Implementation of a personalized home strengthening and flexibility program
- Possible recommendation of a semi-rigid orthotic
- Ice therapy (20 minutes on and 1 hour off)
- Possible recommendation of prescribed or over-the-counter anti-inflammatory medications (taken with food)
- Temporary use of an elastic sleeve with a lateral stabilizing pad for the knee.
For more information on Patellofemoral Syndrome, or to schedule an appointment with Dr. Dubin, call 617-471-2444.
Note: Consult with a doctor before conducting the above exercise routines.

