 Iliotibial band friction syndrome is a common knee injury afflicting athletes who participate in sports that involve repetitive flexion (knee bends) and extension (knee straightens out), such as cycling and running. The first symptom of iliotibial band friction syndrome is a mild ache on the outside of the knee. Typically this ache does not hinder training, and the discomfort disappears before the next training session. If training continues without proper treatment, the mild ache the outside of the knee may progress to an intense burning or stabbing sensation, which can then radiate to the outside of the thigh and calf. At this later stage of the injury, the speed and distance of the training runs are decreased because of extreme discomfort with flexion of the knee, and the intensity of the pain may eventually force the athlete to stop training.
Iliotibial band friction syndrome is a common knee injury afflicting athletes who participate in sports that involve repetitive flexion (knee bends) and extension (knee straightens out), such as cycling and running. The first symptom of iliotibial band friction syndrome is a mild ache on the outside of the knee. Typically this ache does not hinder training, and the discomfort disappears before the next training session. If training continues without proper treatment, the mild ache the outside of the knee may progress to an intense burning or stabbing sensation, which can then radiate to the outside of the thigh and calf. At this later stage of the injury, the speed and distance of the training runs are decreased because of extreme discomfort with flexion of the knee, and the intensity of the pain may eventually force the athlete to stop training.
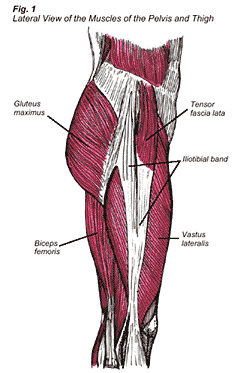
The iliotibial band (also called the “I.T. band”) is located on the outside of the thigh. It is a lateral thickening of the fascia that surrounds the thigh. (Fascia is a sheath-like tissue that surrounds muscles and muscle groups). The I.T. band travels from the outside of the hip, thigh, and knee, and inserts below the knee on a bump on the leg bone called Gerdy’s tubercle. The gluteus maximus muscle (buttocks muscle) and the tensor fascia lata muscle (just outside the pelvis) attach to the back and front of the iliotibial band respectively (Fig. 1). The gluteus maximus and tensor fascia lata muscles contract and increase tension on the iliotibial band, aiding in stabilization of the hip and knee joint.
Iliotibial band friction syndrome can be explained by describing what goes on with the surrounding muscles when the knee flexes and extends. When the knee flexes approximately 30 degrees, tension acts on the I.T. band, causing it to be pulled backwards over the lateral femoral condyle (an outgrowth of the thigh bone on the outside of the knee) (Fig. 2). Conversely, when the knee extends, tension on the I.T. band causes the band to move forward over the lateral femoral condyle (Fig. 3). A thin bursa, or a fluid filled sac, separates the iliotibial band from the lateral femoral condyle, acting to decrease friction between these neighboring structures. Repetitive flexion and extension of the knee will cause inflammation of the bursa and iliotibial band or irritation of the periosteum of the lateral femoral condyle, resulting in iliotibial band friction syndrome.
Checklist for the Prevention of Iliotibial Band Friction Syndrome:
- Avoid training on uneven surfaces, as the down leg would be predisposed to the development of iliotibial band friction syndrome.
- Avoid adding many down hills to training runs. Downhill running will fatigue the quadricep musculature, muscles on the front of the thigh, which are the main stabilizers of the knee. The repetitive flexion and extension of the knee, combined with overstrain of the iliotibial band due to fatigued quadricep musculature, will predispose a runner to the development of iliotibial band friction syndrome.
- Change sneakers every 250-400 miles, approximately every 3-4 months, when they have lost 40% of their shock absorbing abilities. Marathon runners should alternate two pair of sneakers during their training program.
- Slowly increase training mileage.
- Train at an appropriate intensity. Long training runs should be conducted at an aerobic capacity where you can talk and run at the same time. Training at higher intensities will lead to lactic acid production, which will fatigue the muscles and increase the chance of injury. A heart rate monitor may be a useful training device.
- A semi-rigid orthotic may be useful for athletes who have excessively flat feet or high arches, both of which can increase the risk of developing iliotibial band friction syndrome.
- After a run, stretch and then ice the outside of the knee for 20 minutes.
- Include a proper strength training program to improve stabilization of the knee joint.
- For runners, cross training with swimming, biking and the elliptical machine will maintain aerobic capacity and help in the prevention of iliotibial band friction syndrome.
Treatment of iliotibial band friction syndrome at Dr. Dubin’s office would consist of:
- Specific deep tissue procedures to the muscles of the thigh and leg to free up soft tissue motion
- Adjustments of the low back, hip, knee and foot to free up joint motion
- Ultrasound and electric muscle stimulation combotherapy to restore normal muscle tone, decrease pain, and absorb scar tissue
- Implementation of a personalized home strengthening and flexibility program
- Recommendation of a semi-rigid orthotic for individuals with flat feet or high arches.

