ABSTRACT:
Iliotibial band friction syndrome (ITBFS) is an inflammatory, non-traumatic, overuse injury of the knee affecting predominantly long-distance runners. A home exercise program that includes a flexibility and strength conditioning routine and modified training recommendations can aid in the treatment and prevention of further injury. Most cases of ITBFS can be treated successfully with conservative therapy. Recalcitrant cases of ITBFS may require other interventions such as cortisone injections and/or surgery.
Iliotibial Band Friction Syndrome
Running has increased in popularity for cardiovascular fitness and sport over the last decade (1,2,3,4). It has been estimated that approximately 30 million Americans run for exercise (5). However, it has also been projected that one-half to two-thirds of those runners may sustain a non-traumatic repetitive strain injury at least once (5,6). Iliotibial band friction syndrome (ITBFS) is an inflammatory, repetitive strain injury to the knee that is particularly common in long distance runners (1,7,8,9,10). ITBFS may be caused by a multitude of factors including training errors, worn out running shoes, and/or lower leg misalignments (1,4,11,12,13,14,15,16). The main symptom of ITBFS is a sharp pain on the outer aspect of the knee that can radiate into the outer thigh or calf (17,18,19). Knee pain usually occurs at a particular distance of each training run, probably due to muscle fatigue (1,12), and is more pronounced shortly after the foot contacts the ground surface (20). Attempting to run throughout the pain will intensify the symptoms, eventually causing the athlete to shorten his stride or walk. The frustrated athlete, who may be training for a race, will not be able to progress his mileage appropriately. However, the despondent runner may be unreceptive to advice to temporarily discontinue running and initiate therapy, resulting in a more severe grade of injury. Pain may now be present with walking, exacerbated by walking up or down stairs, and a stiff-legged gait may be acquired to relieve symptoms (21). Based on clinical experience and as a recreational runner, I have identified several reasons why most athletes are unwilling to temporarily discontinue running: it is a time-efficient exercise; genuine friendships are formed in group training; no other cardiovascular exercise can beat the “runner’s high”; and the fear of not attaining his or her training goal. My experience and research studies show conservative therapy to be extremely successful in the treatment of ITBFS (8,22). A proper treatment protocol should include the following: inflammation reduction, pain-free training modification, flexibility and endurance strength training of the muscles surrounding the pelvis and thigh, and correction of faulty training habits (1,2,7,8,9,10,11,12,13,23,24).
The treating physician should have an understanding of the anatomy of the iliotibial tract, surrounding musculature of the outer thigh and pelvis, the extrinsic and intrinsic risk factors that predispose long distance runners to ITBFS, and the biomechanics of the ankle, tibia and knee during the stance phase of gait.
Anatomy of the Iliotibial Tract
Fascia is a sheath-like tissue that surrounds muscles and muscle groups. The fascia lata surrounds the hip and thigh. The iliotibial tract (ITT) is a lateral thickening of the fascia lata, originating from the iliac crest of the pelvis. The ITT continues down the outer third of the thigh, at the femur bone, passing over a protuberance called the greater trochanter. At the level of the greater trochanter, fibers from the gluteus maximus (GM) and Tensor fascia lata (TFL) musculature merge with the ITT posteriorly and anteriorly, respectively. Located between the ITT and greater trochanter is a bursa, a fluid filled sac that functions to decrease friction between two adjacent structures. The ITT attaches superficially to the fascia of the vastus lateralis musculature, and through passage of the intermuscular septum to the linea aspera, a linear ridge on the posterolateral aspect of the femur. As the ITT approaches the knee joint, it passes over a protuberance on the outer aspect of the femur, the lateral femoral epicondyle (LFE). A thin layer of fatty tissue is located between the ITT and LFE. As the ITT approaches the knee joint it splits into two structures, the iliopatellar band and a distal extension of the ITT. The distal extension of the ITT crosses the knee joint and attaches to Gerdy’s tubercle, a bump located on the proximal outer aspect of the tibia. The iliopatellar band migrates medially to join with the lateral retinaculum, a sheath-like tissue that attaches to the outer aspect of the patella (Figure 1,16,19,20,25,26,27,28,29,30,31). The distal extension of the ITT provides lateral stabilization to the knee joint through its attachment to the distal femur and the proximal tibia; the iliopatellar branch of the ITT aids in decelerating medial glide of the patella and leg flexion (32).
To properly diagnose, treat, and prevent ITBFS, a physician should understand the biomechanics of the ankle, tibia, and knee joint that this area undergoes during a typical running gait, and how these movements dynamically affect the ITT.
Lower Leg Biomechanics with Running
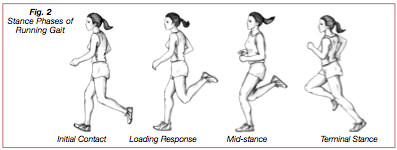
Gait can be separated into two phases: the stance and swing phases. This discussion will focus on the stance phase, as it directly relates to ITBFS. During the stance phase, the foot contacts and adapts to the ground surface; during the swing phase, the leg accelerates forward and prepares for ground contact. The stance phase consists of initial contact, loading response, mid-stance, and terminal stance (33) (Figure 2). The ankle joint, tibia, and knee joint move in synchronicity during the individual stance phases, changing the lower extremity into a rigid lever for initial ground contact and toe-off, or a mobile shock absorber from loading response and into early mid stance (34).
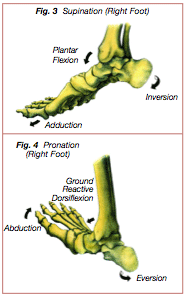
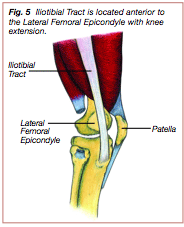
Two tri-planar movements are particular to the ankle joint during the stance phase, supination and pronation. The ankle assumes a supinated position for stability during initial contact and in preparation for toe-off. Supination consists of calcaneal inversion (the heel is turned inwards), plantar flexion (the toes approach the ground surface) and adduction of the forefoot (the toes point toward the midline) (Figure 3). Ankle pronation occurs throughout loading response and into early mid stance, transforming the foot and ankle into a supple mobile adaptor that is efficient in absorbing ground reactive forces. Ankle pronation consists of eversion of the calcaneus (the heel turns outward), ground reactive dorsiflexion (the tibia moves forward over the foot) and abduction of the forefoot (the toes and forefoot turn away from the midline) (Figure 4) (2,35).
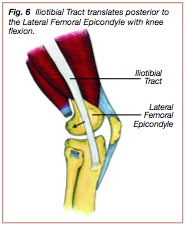
During initial contact the knee is flexed approximately 21 degrees (36), the ITT should be located anterior to the LFE, and the ankle is supinated (Figure 5). Throughout loading response and early midstance, the ankle pronates, the tibia internally rotates, the knee joint flexes beyond 30 degrees, and the ITT translates posterior to the LFE (Figure 6). From early midstance and continuing into terminal stance the ankle re-supinates, the tibia externally rotates and the knee re-extends (33).
It has been proposed that ITBFS is secondary to repetitive knee movement through an impingement zone of 30 degrees of leg flexion (9,10,17). This injury is most common in long distance runners because the activity involves repetitive leg flexion and extension approximately 800 times per mile (37,38). The onset of pain associated with ITBFS will cause an athlete to shorten his stride, thereby limiting leg flexion and minimizing friction of the ITT over the inflamed fatty tissue and periosteal layer of the LFE. This
altered gait will temporarily allow the athlete to continue running, but may exacerbate the condition. A study performed on athletes who had acute or sub-acute clinical symptoms for ITBFS revealed MRI findings of fluid accumulation in the fatty tissue deep to the ITT (17,39,40). Secondary bursa or thickening of the ITT may be more common in chronic stages of ITBFS (41).
Repetitive flexion and extension of the leg through the 30 degree impingement zone may be one risk factor; however the causes of ITBFS are multifaceted. Other risk factors include training errors and structural misalignments.
Training Errors and Risk Factors for ITBFS
Training errors are contributory to most overuse running injuries. Properly progressed training programs allow the supporting structures of the pelvis and knee to adapt to increased stresses. Inappropriately increasing the intensity, duration, and frequency of the training runs, as well as incorporating hills on the training routes too soon, may overload the supporting structures of the knee, eventually leading to injury (2,8,9,11,12).
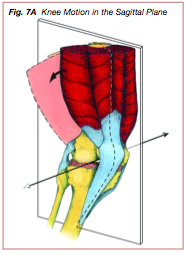
Structural misalignments that cause altered movement patterns of the ankle, tibia and knee joint can also be contributory to ITBFS. Knee movement occurs in 3 planes of reference: the sagittal plane, frontal plane, and transverse plane. Flexion and extension of the leg occur in the sagittal plane (Figure 7A). Frontal plane movements include varus (gapping of the lateral aspect of the knee joint) (Figure 7B), as well as adduction of the lower extremity towards the midline. Internal rotation of the tibia on the fixed femur takes place in the transverse plane (Figure 7C). Excessive repetitive movement patterns of the knee occurring in the sagittal, frontal, and transverse planes are risk factors for ITBFS (17,18,20,21).
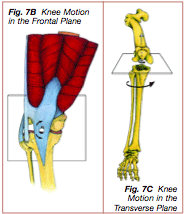
Studies have suggested two factors that lead to excessive adduction of the stance leg in the frontal plane, causing increased tension of the ITT: weakness of the muscles that abduct and support the pelvis, and running on cambered (arched) surfaces (20). Contraction of the gluteus medius, GM, and TFL occur predominately during the first 35% of stance (9). Long distance runners with ITBFS have weaker hip abduction strength in the affected leg compared with their unaffected leg (10). Fatigue and weakness of the GM, TFL, and gluteus medius may occur later during a run, resulting in an altered “Trendelenberg gait,” raised ipsilateral hip, and increased frontal plane adduction of the thigh and leg (1,42) (Figure 8). This modified gait has been shown to increase tension on the ITT and is a risk factor for ITBFS (1,20).
Pronounced adduction of the stance leg due to muscle fatigue leads to increased tension on the ITT that may initiate or exacerbate symptoms related to ITBFS.
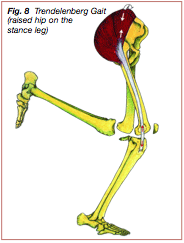
Excessive internal rotation of the tibia in the transverse plane can also be caused by structural misalignments and can contribute to ITBFS. Anatomical misalignments such as rearfoot varus, forefoot varus, and pes planus may cause excessive or prolonged pronation of the ankle joint throughout the stance phase of gait. Abnormal pronation of the ankle joint may cause greater than normal internal rotation of the tibia, accompanied by increased tension on the ITT at its insertion point on Gerdy’s tubercle during each foot strike, predisposing to injury (1,12,38,43,44,45) (Figure 9).
Risk Factors for ITBFS
Extrinsic risk factors may include:
- Worn out running shoes. A sneaker loses approximately 50% of its ability to absorb ground reactive forces after 300-500 miles (14). The more worn out the shoe, the more ground reactive forces are transferred to the knee.
- Training programs that increase mileage or incorporate hills inappropriately. Weekly mileage should not be increased more than 5-10% per week to allow for adaptation of the muscles, tendons, ligaments and bone to increased stress (46,47,48).
- Running at an improper pace. Placing too much strain on untrained legs may lead to fatigue and injury. Long runs to improve aerobic conditioning should be slow, at 65-70% maximum heart rate. Anaerobic threshold training can be conducted with shorter runs at 85-100% maximum heart rate (46).
- Running on a cambered surface or slippery surface (11).
Intrinsic risk factors may include:
- Bow leg/genu varum (49)
Rearfoot and forefoot varum (50)
- Pes cavus/high arch. A pes cavus foot has limited ability in absorbing ground reactive forces, placing more stress on the knee joint.
- A prominent LFE and tight IT and TFL.
- Weak gluteus medius, GM and TFL (42).
- Tightness and weakness in the Quadriceps, ITT and lateral retinaculum. This may lead to excessive lateral tracking of the patella and decreased deceleration forces acting on leg flexion, leading to increased stress on the lateral stabilizing structures of the knee joint (47,51).
Diagnosing ITBFS
A physician can diagnose ITBFS and discover internal and external risk factors for the condition through a detailed history and physical examination. A history should include the following questions: What are your current symptoms? When did you first notice the injury? How have you progressed the frequency, duration and intensity of your weekly training runs? Do your training routes include hills or cambered surfaces? How old are your running sneakers? What are your training goals?
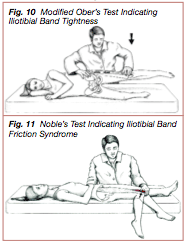
Two orthopedic tests that aid the doctor in diagnosing ITBFS are the Modified Ober’s test (Figure 10) (42,52) and Noble’s test (Figure 11) (15,17,52). The Modified Ober’s test is an assessment tool for evaluating tightness of the ITT and TFL. Initially the patient lies on the non-injured side. The doctor raises the upside hip and thigh into slight abduction, extends the thigh, and then allows the thigh to drop vertically into adduction. The doctor should stabilize the pelvis and thigh with one hand to prevent flexion of the pelvis and internal rotation of the thigh, movements that may lead to false negative findings. The Modified Ober’s test is positive for a tight ITT and TFL if the thigh does not descend to or beyond 10 degrees of the horizontal plane.
Noble’s test can be utilized to differentiate between ITBFS and other conditions that refer pain to the outside of the knee, such as bicipital tendonitis, popliteus tendonitis, lateral collateral ligament strain, lateral meniscal tear or cyst, and osteoarthritis (53,54,55,56,57, 58). The patient is instructed to lie on his back with his leg hanging off the side of the bench and his knee flexed to 90 degrees. The doctor places his thumb over the LFE and instructs the patient to extend his leg. As the patient extends his leg to approximately 30 degrees, the ITT translates anteriorly under the doctor’s thumb. If the patient complains of lateral knee pain that is similar to pain present while running, Noble’s test is positive for ITBFS.
The Creak test (17) is analogous to Noble’s test. During this orthopaedic test the athlete is standing and instructed to transfer his weight to the fully extended injured leg. He is then instructed to flex the injured leg to approximately 30 degrees. As the leg flexes to 30 degrees, the ITT would track over and posterior to the LFE. If lateral knee pain is present at approximately 30 degrees of leg flexion, the test is positive for ITBFS.
Further examination should include a strength and flexibility assessment of the musculature surrounding the thigh and pelvis, and observation of the athlete’s lower extremity biomechanics with standing and walking.
Therapies
Initial goals of therapy are to reduce swelling and inflammation. Pain-free modified training can then be implemented to improve strength and flexibility of the hip, thigh, and calf musculature, as well as cardiovascular fitness. The end goal is to return the athlete to a pain-free running routine. Grading the injury helps to determine the plan of treatment (7,43).
Grades of Iliotibial Friction Injuries and Phases of Tissue Repair and Treatment
Grade 1
Pain does not occur during normal activity, but generalized pain is felt about 1 to 3 hours after sport-specific training has ended. Tenderness usually resolves within 24 hours without intervention.
Grade 2
Minimal pain is present towards the end of a training run; performance is not affected. Appropriate treatment may be necessary to prevent a grade 3 injury.
Grade 3
Pain is present at an earlier onset of training, and interferes with the speed and duration of a training session. Treatment and training modification are necessary to prevent a grade 3 injury from progressing to a grade 4 injury.
Grade 4
Pain restricts training and is also noticeable during activities of daily living; the athlete can no longer continue sport-specific training. Low-impact training, such as swimming, running in a pool, and biking, can be implemented for cardiovascular fitness and aggressive muscu- loskeletal therapy can reduce the severity of the injury. The goal of therapy is to reduce inflammation and restore strength and flexibility of the hip and thigh musculature, allowing for the athlete to return to pain-free sport-specific training.
Grade 5
Pain interferes with training as well as activities of daily living. Aggressive therapy is required and surgery may be necessary. (Source: 7,43)

Appropriate treatment of a grade 1 or grade 2 ITBFS injury would consist of:
- Manual adjustments to the ankle and foot, as well as medial glide mobilization of the patella to free up joint motion and improve tracking of the patella (45).
- Deep tissue procedures, such as the Graston Technique (manual therapy that utilizes specially designed devices) and Active Release Technique (a patented manual therapy technique), to break up scar tissue and restore soft tissue motion (59). There is considerable clinical evidence to support the effectiveness of deep tissue procedures in treatment of strain/sprain injuries (60,61). A home exercise program for myofascial release therapy can be taught on a foam roller (Figure 12).
- Ultrasound and electric muscle stimulation combination therapy to restore normal muscle tone, help in the healing process, and reduce pain (50,62). Iontophoresis with dexamethasone is also a useful modality to decrease inflammation (63).
- Inflammation reduction by taking nonsteroidal anti-inflammatory medications per prescription, and applying a cold pack to the lateral aspect of the knee 20 minutes on/one hour off, repeated throughout the day.
- Implementation of a strength training program for the gluteus medius, GM, and quadricep musculature. Exercises should include squats, standing hip abduction, and supine floor bridges with alternating leg lifts (Figures 13 A-C). Strengthening the gluteus musculature has been shown to be instrumental in returning athletes to pain-free running (10,51). Strengthening exercises should be progressed with no or little discomfort (64). When pain free training resumes, it is my opinion that a leg workout can be included once a week, with at least 48 hours rest before or after a long run.
- Stretching routine. I have found that a 15-20 minute flexibility routine with a resistance band helps in decreasing delayed onset muscle soreness, as well as improving flexibility through hysteresis/creep. The flexibility routine should include stretching of the hamstrings, quadriceps, adductors, ITT, and external rotators of the thigh (65,66,67). Longer stretching (30-60 seconds), with short intermittent contractions of the antagonist, has been shown to be one of the best mobilization techniques for a painful muscle/tendon (11).
- A recommendation to change running shoes every 300-500 miles of use, at which point the shoe loses 50% of its shock absorption capability (8,14).
- A recommendation to use appropriate arch supports as necessary. A runner with pes planus will usually overpronate, leading to increased internal rotation of the tibia, a risk factor for ITBFS. A good sneaker with a firm heel counter and an inside arch support will help correct overpronation. If necessary a semirigid orthosis with a medial arch support no higher then 5/8 inch can be utilized to further control pronation. A runner with pes cavus has limited pronation and poor shock-absorbing capabilities. The high-arch runner should get a sneaker with good cushioning; if necessary a semirigid orthosis or cushioned liner can be added (1,8).
- Recommendation for appropriate training limits. For marathon runners, initially a training base of four miles at 65%-75% maximum heart rate needs to be established. Later, a progressive training schedule should be followed that allows for adaptation of the supporting structures of the knee to withstand future increased stress loads. Long training runs, usually done on the weekend, should be limited to a pace that requires 65-75% maximum heart rate to improve aerobic capacity. During the week, a shorter 4-8 mile interval run at 85-90% maximum heart rate is recommended to improve anaerobic capacity. Hill training should be added gradually because of the increased load placed on the knee joint. The average marathon training schedule consists of 3 shorter runs during the week, and 1 longer run on the weekend. Total mileage should not be increased by more then 10% per week (33,46,50).

Early therapy and intervention (as above) are important to prevent a grade 3 ITBFS injury from progressing to a grade 4 or 5 injury. In the early stages of a grade 3 injury, one week of activity modification from the offending training regimen is recommended, as well as treatment procedures similar to those used to treat a grade 1 or 2 injury. Modified activity with swimming, running in the pool, bicycling, or an elliptical machine would be useful in maintaining aerobic fitness and allow for proper healing. Treating a more advanced grade 3 or grade 4 ITBFS injury would involve a longer bout of modified activity and rest from an offending activity, and a slower progression of weight training and stretching (68,69,70).
Chronic ITBFS may not always resolve with conservative therapy. In recalcitrant ITBFS, other treatment methods may need to be considered, such as steroid injection therapy and surgical procedures. Steroid injections, used judiciously, have been shown to reduce symptoms and inflammation (1,11,12,13). Steroid injection therapy should be followed by a properly progressed strength, flexibility and car- diovascular program to restore function before training resumes. Surgery should only be considered if all other means of therapy fail and the athlete is not willing to give up his sports activity (23). One type of surgery involves lengthening of the ITT at the level where the friction accumulates and typically involves two small incisions. The first incision is in the posterior fibers of the ITT that lie over the LFE when the leg is flexed to 30 degrees. The second incision is placed in the anterior fibers of the ITT proximal to the first incision, and is a “Y” shape to allow for maximal lengthening (1,9). In a study by Holmes et al., open release-excision, a surgical procedure involving removal of an ellipse of tissue that abrades the LFE, was found to be a safe and effective surgical procedure (71).
Conclusion
ITBFS is a common non-traumatic overuse injury that is particularly common in long distance runners. Certain biomechanical malalignments, such as rearfoot varus; forefoot varus; genu varum; pes cavus; a prominent LFE; weak GM, gluteus medius and Quadriceps musculature; and tight TFL, ITT, and lateral retinaculum predispose runners to ITBFS. The risk of ITBFS can be reduced if athletes follow a properly progressed training program that allows for adaptation of the structures supporting the pelvis, thigh and knee. To prevent injury, these athletes should incorporate proper footwear, semirigid orthosis as necessary, a lower body flexibility and strength training routine, and cross training into their workouts.
ITBFS can usually be treated successfully with a conservative rehabilitation program that includes modified training and a flexibility and strength home exercise program. When the athlete can run 3-4 miles pain-free on a treadmill, he can progress his training program carefully to prevent re-injury. Sometimes ITBFS is resistant to conservative therapy and a cortisone injection or surgery may need to be considered as alternative treatment options. Surgery, when necessary, may involve lengthening the ITT and removing a section of the posterior aspect of the ITT that is impinging on the LFE.
References
- Anderson GS. Iliotibial Band Friction Syndrome. The Australian Journal of Science and Medicine in Sport 1991; 81-83.
- Newell SG, Bramwell ST. Overuse Injuries to the Knee in Runners. The Physician and Sportsmedicine 1984; 12(3):80-92.
- Wen DY, Puffer JC, Schmalzried TP. Injuries in Runners: A Prospective Study of Alignment. Clinical Journal of Sports Medicine 1998; 8:187-194.
- Taunton JE, Ryan MB, Clement DB, McKenzie DC, Lloyd-Smith DC, Zumbo BD. A retrospective case-contol analysis of 2002 running injuries. British Journal of Sports Medicine 2002; 36:95-101.
- Kaufman KR, Brodine SK, Shaffer RA, Johnson CW, Cullison TR. The Effect of Foot Structure and Range of Motion on Musculoskeletal Overuse Injuries. American Journal of Sports Medicine 1999; 27(5):585-593.
- Brill PA, Macera CA. The Influence of Running Patterns on Running Injuries. Sports medicine 1995; 20(6):365-368.
- Schwellnus MP, Theunissen L, Noakes TD, Reinach SG. Anti-inflammatory and combined anti-inflammatory/ analgesic medication in the early management of iliotibial band friction syndrome. S Afr Med J 1991; 79:602-606.
- Barber FA, Sutker AN. Iliotibial Band Syndrome. Sports Medicine 1992; 14(2):144-148.
- Orchard JW, Fricker PA, Abud AT, Mason BR. Biomechanics of Iliotibial Band Friction Syndrome in Runners. American Journal of Sports Medicine 1996; 24(3):375-379.
- Fredericson M, Cookingham CL, Chaudhari AM, Dowdell BC, Oestreicher N, Sahrmann S. Hip Abductor Weakness in Distance Runners with Iliotibial Band Syndrome. Clinical Journal of Sport Medicine 2000; 10:169-175.
- Dahan R. Rehabilitation of Muscle- Tendon Injuries to the Hip, Pelvis, and Groin Areas. Sports Medicine and Arthroscopy Review 1997; 5:326-333.
- McNicol K. Iliotibial Tract Friction Syndrome in Athletes. Canadian Journal of Applied Sport Sciences 1981; 6(2): 76-80.
- Gunter P, Schwellnus MP. Local corticosteroid injection in iliotibial band friction syndrome in runners: a randomized controlled trial. British Journal of Sports Medicine 2004; 38:269-272.
- Messier SP, Edwards DG, Martin DF, Lowery RB, Cannon DW, James MK, Curl WW, Read HM Jr., Hunter DM. Etiology of iliotibial band friction syndrome in distance runners. Medicine and Science in Sports and Exercise 1995; 27(7):951-960.
- Noble C. Iliotibial band friction syndrome in runners. American Journal of Sports Medicine 1980; 8(4):232-234.
- Kwak SD, Ahmad CS, Gardner TR, Grelsamer RP, Henry JH, Blankevoort L, Ateshian GA, Mow VC. Hamstrings and Iliotibial Band Forces Affect Knee Kinematics and Contact Pattern. Journal of Orthopaedic Research 2000; 18:101-108.
- Kirk KL, Kuklo T, Klemme W. Iliotibial Band Friction Syndrome. Orthopedics?(orthobluejournal.co m) 2000; 23(11) 1209-1215.
- Noble AH, Hajek MR, Porter M. Diagnosis and Treatment of Iliotibial Band Tightness in Runners. The Physician and Sportsmedicine 1982; 10(4):67-74.
- Orvava S. Iliotibial Tract Friction Syndrome in Athletes – An Uncommon Exertion Syndrome on the Lateral Side of the Knee. British Journal of Sports Medicine 1978; 12(2):69-73.
- Birnbaum K, Siebert CH, Pandorf T, Schopphoff E, Prescher A, Niethard FU. Anatomical and biomechanical investigations of the iliotibial tract. Surg Radiol Anat 2004; 26:433-446.
- Renne JW. The Iliotibial Band Friction Syndrome. The Journal of Bone and Joint Surgery 1975; 57A(8):1110-1111.
- Provencher MT, Hofmeister EP, Muldoon MP. The Surgical Treatment of External Coxa Saltans (the Snapping Hip) by Z-plasty of the Iliotibial Band. American Journal of Sports Medicine 2004; 32(2):470-476.
- Martens M, Librecht P, Burssens A. Surgical Treatment of the iliotibial band friction syndrome. American Journal of Sports Medicine 1989; 17(5):651-654.
- Sutker AN, Barber A, Jackson DW, Pagliano JW.Iliotibial Band Syndrome in Distance Runners. Sports medicine 1985; 2:447-451.
- Anderson K, Strickland SM, Warren R. Hip and Groin Injuries in Athletes. American Journal of Sports Medicine 2001; 29(4):521-533.
- Terry GC, LaPrade RF. The Biceps Femoris Muscle Complex at the Knee: Its Anatomy and Injury Patterns Associated with Acute Anterolateral-Anteromedial Rotary Instability. American Journal of Sports Medicine 1996; 24(1):2-8.
- Staubli HU, Rauschning W. Popliteus Tendon and Lateral Meniscus: Gross and Multiplanar Cryosectional Anatomy of the Knee. American Journal of Knee Surgery 1991; 4(3):110-121.
- Brignall CG, Brown RM, Stainsby GD. Fibrosis of the Gluteus Maximus as a Cause of Snapping Hip. The Journal of Bone and Joint Surgery 1993; 75A(6):909-910.
- Doucette SA. The effect of exercise on patellar tracking in lateral patellar compression syndrome. American Journal of Sports Medicine 1992; 20(4):434-440.
- White RA, Hughes MS, Burd, T, Hamann J, Allen WC. A New Operative Approach in the Correction of External Coxa Saltans. American Journal of Sports Medicine 2004; 32(6):1504-1508.
- Gruen GS, Scioscia TN, Lowenstein JE. The Surgical Treatment of Internal Snapping Hip. American Journal of Sports Medicine 2002; 30(4):607-613.
- Terry GC, Hughston JC, Norwood LA. The anatomy of the iliopatellar band and iliotibial tract. American Journal of Sports Medicine 1986; 14(1):39-45.
- Norkin CC, Levangie PK. Joint structure and function: a comprehensive analysis, 2nd ed. Philadelphia: F.A. Davis, 1992:448-458.
- Donatelli RA. The biomechanics of the foot and ankle, 2nd ed. Philadelphia: F.A. Davis, 1996.
- Michaud TC. Foot orthosis and other forms of conservative foot care. Newton MA: Thomas C. Michaud, 1997.
- Swanson SC, Caldwell GE. An integrated biomechanical analysis of high speed incline and level treadmill running. Medicine & Science in Sports & Exercise 2000; 32(6):1146-1155.
- Scott SH, Winter DA. Internal forces at chronic running injury sites. Med Sci Sports Exerc 1990;22(3):357-369.
- Schepsis AA, Jones H, Haas AL. Achilles tendon disorders in athletes. Am J Sports Med 2002;30(2):287-305.
- Sanders TG, Miller MD. A Systematic Approach to Magnetic Resonance Imaging Interpretation of Sports Medicine Injuries of the Knee. American Journal of Sports Medicine 2005; 33(1):131-148.
- Muhle C, Ahn JM, Yeh LR, Bergman GA, Boutin RD, Schweitzer M, Jacobson JA, Haghighi P, Trudell DJ, Resnick D. Iliotibial Band Friction Syndrome: MR Imaging Findings in 16 Patients and MR Arthrographic Study of Six Cadaveric Knees. Radiology 1999; 212:103-110.
- Nemeth WC, Sanders BL. The Lateral Synovial Recess of the Knee: Anatomy and Role in Chronic Iliotibial Band Friction Syndrome. Arthroscopy: The Journal of Arthroscopic and Related Surgery 1996; 12(5):574-580.
- Kendall FP, McCreary EK, Provance PG. Muscles:Testing and Function, 4th edition. Baltimore: William & Wilkins, 1993.
- Sundqvist H, Forsskahl B, Kvist M. A promising novel therapy for Achilles Peritendinitis: double-blind comparison of glycosaminoglycans polysulfate And high-dose indomethacine. Int J Sports Med 1987;(8):298-303
- Smart GW, Taunton JE, Clement DB. Achilles tendon disorders in runners – a review. Med Sci Sports Exerc 1980;12(4):231-243.
- Menetrey J, Fritschy D. Subtalar subluxation in balet dancers. Am J Sports Med 1999;27(2):143-149.
- Smurawa TM. The Endurance Triathlete, Racing and Recovery.
- Scott WN. The Knee. Mosby, St. Louis. MO 1994.
- Martin DE, Coe PN. Better Training for Distance Runners. Illinois: Human Kinetics, 1997.
- LaPrade RF, Meunch C, Wentorf F, Lewis JL. The Effect of Injury to the Posterolateral Structures of the Knee on Force in a Posterior Cruciate Ligament Graft. American Journal of Sports Medicine 2002; 30(2):233-238.
- Reid DC. Sports Injury Assessment and Rehabilitation. New York: Churchill Livingston Inc., 1992.
- Doucetter SA, Child DD. The Effect of Open and Closed Chain Exercise and Knee Joint Position on Patellar Tracking in Lateral Patellar Compression Syndrome. JOSPT 1996; 23(2):104-110.
- Hyde TE, Gengenbach MS. Conservative Management of Sports Injuries. Baltimore, Maryland: Williams & Wilkins, 1997.
- LaPrade RF, Konowalchuk BK. Popliteomeniscal Fascicle Tears Causing Symptomatic Lateral Compartment Knee Pain: Diagnosis by the Figure-4 Test and Treatment by Open Repair. American Journal of Sports Medicine 2005. AJSM PreView published on July 6, 2005 as doi:10.1177/0363546504274144.
- LaPrade RF, Bollom TS, Wentorf FA, Wills NJ, Meister K. Mechanical Properties of the Posterolateral Structures of the Knee. American Journal of Sports Medicine 2005. AJSM PreView published on July 7, 2005 as doi:10.1177/0363546504274143.
- Jones CDS, Keene GCR, Christie AD. The Popliteus as a Retractor of the Lateral Meniscus of the Knee. Arthroscopy: The Journal of Arthroscopic and Related Surgery 1995; 11(3):270-274.
- LaPrade RF, Hamilton CD. The Fibular Collateral Ligament-Biceps Femoris Bursa: An Anatomic Study. American Journal of Sports Medicine 1997; 25(4):439-443.
- Biedert RM, Stauffer E, Friederich NF. Occurrence of free nerve endings in the soft tissue of the knee joint. American Journal of Sports Medicine 1992; 20(4):430-433.
- Bach BR, Minihane K. Subluxating Biceps Femoris Tendon: An Unusual Case of Lateral Knee Pain in a Soccer Athlete. American Journal of Sports Medicine 2001; 29(1):93-95.
- Kvist M, Jarvinen M. Clinical Histochemical and Biomechanical Features in Repair of Muscle and Tendon Injuries. International Journal of Sports Medicine. 1982; (3): 12-14.
- Walker JM. Deep Transverse Frictions in Ligament Healing. The Journal of Orthopaedic and Sports Physical Therapy 1984; 6(2):89-94.
- Brosseau L, Casimiro, Milne S, Robinson VA, Shea BJ, Tugwell P, Wells G. Deep transverse friction massage for treating tendinitis. The Cochrane Collaboration 2005; Volume (2).
- Gum SL, Reddy GK, Stehno-Bittel L, Enwemeka CS. Combined ultrasound, electric muscle stimulation, and laser promote collagen synthesis with moderate changes in tendon biomechanics. Am J Phys Med Rehabil 1997;76(4):288-296.
- Pellecchia GL, Hamel H, Behnke P. Treatment of Infrapatellar Tendinitis: A Combination of Modalities and Transverse Friction Massage Versus Iontophoresis. Journal of Sport Rehabilitation 1994; 3:135-145.
- Cohen ZA, Roglic H, Grelsamer R, Henry JH, Levine WN, Mow VC, Ateshian GA. Patellofemoral Stresses during Open and Closed Kinetic Chain Exercises. American Journal of Sports Medicine 2001; 29(4):480-487.
- Morelli V, Smith V. Groin Injuries in Athletes. American Family Physician 2001; 64(8):1405-1414.
- Heidt RS Jr., Sweeterman LM, Carlonas RL, Traub JA, Tekulve FX. Avoidance of Soccer Injuries with Preseason Conditioning. American Journal of Sports Medicine 2000; 28(5):659-662.
- Mirzabeigi E, Jordan C, Gronley JK, Rockowitz NL, Perry J. Isolation of the Vastus Medialis Oblique During Exercise. American Journal of Sports Medicine 1999; 27(1):50-53.
- James SL, Bates BT, Osternig LR. Injuries to runners. Am J Sports Med 1978;6(2): 40-50.
- Clement DB, Taunton JE, Smart GW. Achilles tendonitis and peritendinitis: etiology and treatment. AM J Sports Med 1984;12(3):179-184.
- Leadbetter WB. Cell matrix response in tendon injury. Clin Sports Med 1992;11(3): 533-579.
- Holmes JC, Pruitt AL, Whalen NJ. Iliotibial band syndrome in cyclists. American Journal of Sports Medicine 1993; 21(3):419-424.
©2006 Dubin Chiropractic
Special thanks to Audrey Mahoney for creating the illustrations.

