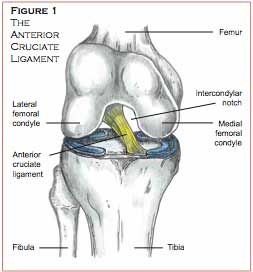
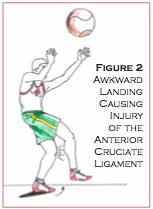
 The anterior cruciate ligament (ACL) is a tough fibrous structure that attaches the tibia (lower leg bone) to the femur (thigh bone) (Figure 1). This ligament helps to stabilize the knee by preventing excessive forward movement of the tibia on the femur. ACL injuries commonly occur in athletes participating in sports such as football, basketball, soccer, and volleyball, where movements such as cutting, pivoting, single leg landing and rapid decelerations are routinely performed. Tearing of the ACL is most commonly caused by landing awkwardly or cutting on a fully extended or slightly flexed leg with the foot turned outward (Figure 2).
The anterior cruciate ligament (ACL) is a tough fibrous structure that attaches the tibia (lower leg bone) to the femur (thigh bone) (Figure 1). This ligament helps to stabilize the knee by preventing excessive forward movement of the tibia on the femur. ACL injuries commonly occur in athletes participating in sports such as football, basketball, soccer, and volleyball, where movements such as cutting, pivoting, single leg landing and rapid decelerations are routinely performed. Tearing of the ACL is most commonly caused by landing awkwardly or cutting on a fully extended or slightly flexed leg with the foot turned outward (Figure 2).
Skiers usually injure the ACL when they catch the inside edge of a ski on ice, causing them to lose control and fall backwards as they hyperflex the knee. The injured athlete may report hearing a “pop” and that it felt like the knee was being stretched apart. Examination of the knee may reveal extensive swelling around the knee joint, loss of full extension of the knee and an inability of the athlete to bear weight on the injured leg. Manual testing may reveal excessive forward movement of the tibia on the femur.
 Once the athlete is diagnosed with an ACL injury, the first step is to decide whether to undergo surgery to reconstruct the torn ligament, or to rehabilitate the knee without surgery. ACL reconstructive surgery would be recommended for athletes who continue to suffer from repetitive bouts of the knee giving away, or for those athletes who want to return to a highly competitive sport level. Athletes deciding not to have reconstructive surgery may be able to return to an active lifestyle after completing a rehabilitation program; however, they must learn to modify their activities to accommodate for the compromised stability of the knee due to the lost check-rein function of the ACL.
Once the athlete is diagnosed with an ACL injury, the first step is to decide whether to undergo surgery to reconstruct the torn ligament, or to rehabilitate the knee without surgery. ACL reconstructive surgery would be recommended for athletes who continue to suffer from repetitive bouts of the knee giving away, or for those athletes who want to return to a highly competitive sport level. Athletes deciding not to have reconstructive surgery may be able to return to an active lifestyle after completing a rehabilitation program; however, they must learn to modify their activities to accommodate for the compromised stability of the knee due to the lost check-rein function of the ACL.
Pre-operative rehabilitation is important for those athletes who choose to undergo surgical reconstruction. The main goals of the pre-operative rehabilitation protocol are to reduce swelling around the knee joint, and to restore full range of motion and functional strength to the injured limb. The pre-operative rehabilitation phase prepares the patient physically and mentally for both the surgery and the postoperative rehabilitation program.
Post-operative rehabilitation begins immediately after surgery. The most important goals in the first two weeks are to reduce swelling and restore full range of motion of the knee in extension and flexion. Once range of motion is restored and swelling is minimized, the progression of the post-operative program depends on the patient’s determination, level of swelling and pain, and the clinician’s knowledge of the normal biological progression of healing of the reconstructed ligament. Some athletes progress rapidly in the post-operative phase of rehabilitation and may begin sport-specific training at a low intensity level in two to three months. However, full functional rehabilitation of the reconstructed ACL may not occur until six to 12 months post-operatively. The therapist must be careful on the progression of the rehabilitation exercises and on the timetable for returning the athlete to their particular sport. An accelerated rehabilitation program under a controlled environment allows the athlete to return to sport sooner, without increasing the risk of complications.
Origin and Insertion Points of the Anterior Cruciate Ligament
The bottom of the femur consists of the medial and lateral femoral condyles, circular bony protuberances that are separated by an intercondylar notch. The top of the tibia consists of the medial and lateral tibial plateaus, flat slightly concave surfaces that articulate with the respective femoral condyles. The anterior cruciate ligament originates from the posterior outer aspect of the intercondylar notch and proceeds anteriorly, where it inserts onto the outside edge of the medial tibial plateau (see Figure 1).
Graft Tissue Healing Post-Surgery
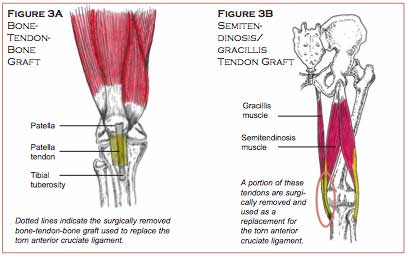
In athletes, a torn anterior cruciate ligament is typically removed and replaced by their own tissue that is similar in length and strength. The two most common self-tissue grafts are the bone-tendon-bone (specifically, tibial tuberosity bone – patella tendon – patella bone graft) (Figure 3A), and the hamstring tendon graft (specifically, the tendons of the inside hamstring muscle [semitendinosis], and adjacent groin muscle [gracillis]) (Figure 3B). The selected graft tissue would be surgically placed in the anatomical location of the previous ACL and then secured by interference screws.
Both types of grafts have advantages and disadvantages. The surgeon selects the appropriate type of surgery based on the patient’s sport and the movements most frequently used.
A study by Rodeo et al evaluated tendon-to-bone healing in a dog model and found that a firm attachment of tendon to bone occurred at 12 weeks post-surgery. At two weeks post surgery there was still no continuity between the graft tendon and the insertion point in the bone. At four weeks there was minimal continuity between tendon and bone. At eight weeks there was considerably improved continuity between tendon and bone. After 12 weeks the tendon graft was safely secured to the surrounding bone, at which point failure of the graft-insertion point was minimal.
Based on the results of the above study, from zero to four weeks post-surgery therapy should focus on decreasing inflammation and restoring full range of motion of the knee. Swimming, stationary cycling, isometric contraction exercises, and other low-force muscle integrating techniques can be implemented in the earlier stages of rehabilitation. If the patient experiences pain, swelling or decreased range of motion of the knee, the inflammation should be reduced, range of motion restored, and the intensity of the rehabilitation phase should be slowed down. During the 12-week healing period, exercise selection should be carefully monitored by a skilled therapist to reduce the risk of complications.
Rehabilitation of the Knee: Decrease Swelling and Restore Range of Motion
Rehabilitation after ACL reconstruction surgery should initially focus on decreasing inflammation and restoring normal range of motion. Every patient heals differently; the progression of the rehabilitation program should be customized to the athlete and progressed to their tolerance.
Initially decreasing inflammation around the knee joint using ice, compression, and elevation is feasible with a couple of icepacks, an ace bandage, and pillows to prop the leg up. Ice therapy should be maintained 20 minutes on and one hour off, multiple times per day. Ankle pumps (flexion and extention of the foot) with the leg elevated can be conducted five minutes per hour to further reduce swelling. A Cryo-Cuff, if available, is a more advanced method of decreasing inflammation. The Cryo-Cuff can be wrapped around the knee and filled with ice water. A cooler of ice water is attached by tubing to the CryoCuff and can be used to replace the old water in the cuff with ice cold water every hour. Anti-inflammatory medication is also useful in reducing swelling around the knee joint.
The next couple of steps of the post-operative phase should be conducted to the patient’s tolerance.
The patient should use crutches following the first two days post-surgery, with minimal weight bearing. Additional weight may be applied to the injured leg, with crutches, as tolerated. By the end of the first week, the patient may ambulate without the support of crutches if a normal walking gait cycle with full weight bearing can be sustained with no noticeable instability. The patient should be able to ambulate without crutches six to seven days post-operatively.
Restoring full range of motion of the injured knee, particularly in extension, should be a priority in the first two weeks post-surgery. After the first week of post-operative rehabilitation, the patient should be able to fully extend the leg and flex the leg to 110 degrees. At this point, full extension is the most important goal; flexion of the knee improves steadily as swelling around the knee joint decreases. If full extension of the knee is not restored within two weeks post-surgery, scar tissue may develop in the joint, preventing the restoration of full knee extension.
The continuous passive motion machine (CPM), an electrical motor-driven device, may be used in the hospital immediately following recovery from surgery. This machine has shown promise in helping to restore normal motion and flexibility of the injured leg. The CPM supports the leg while moving it from full extension to a progressively set degree of flexion. There is a ten-second pause at the end of each movement, during which time the patient will isometrically contract the quadriceps (front thigh muscles).
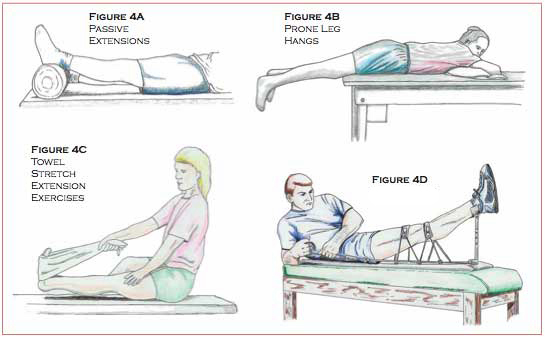
After the patient is released from the hospital, a specific series of exercises (provided by a trained therapist) should be done as often as possible to restore full range of motion of the knee in extension. Passive extensions (Figure 4A) and weighted extensions and prone leg hangs (Figure 4B) are useful exercises for restoring extension of the knee. During passive extensions, the patient can lie on the back with the heel propped up on pillows. Once the leg is relaxed in extension, the patient can periodically contract the quadricep musculature to push the knee further into extension. The patient then holds the quadracep contraction for five seconds, then returns to relaxed extension. This exercise should be done for 15 minutes and repeated every waking hour. If extension is not achieved this way, the patient may progress to weighted extension exercises by placing a five to ten pound weight just above the knee and following a similar procedure as passive extensions. The patient should be instructed to perform this exercise for ten minutes, taking the weight off for one minute and repeating multiple times during the day. Prone leg hangs (Figure 4B) can also aid in restoring extension of the knee. Have the patient lie on the stomach with the knee just past the edge of the table or bench with the knee in full extension; use a weight if struggling with full extension. The patient should perform this exercise for ten minutes, by gently flexing and extending the knee and repeating multiple times per day.
Towel stretch extension exercises (Figure 4C) can be incorporated if the above exercises are not restoring extension appropriately. The patient sits on a bench, places a towel around the foot of the injured leg, and applies tension to the towel to dorsiflex the foot, pulling the toes backward. The patient then raises the heel off of the ground to bring the knee into extension while placing the other hand on the thigh to stabilize the leg.
The patient would lie down on the back with the ankle raised and secured into a heel rest; a pad would be placed above and below the knee joint. These pads are secured by ropes passing through a ratchet system that would be tightened to force the knee into full extension (Figure 4D).
A normal gait cycle depends on a person’s ability to lock the knee in full extension while weight bearing. The following resistive tubing exercise can aid in accomplishing this goal. Resistive tubing can be secured above the standing patient’s knee cap and anchored to a bench behind the patient; the resistive force of the tubing will promote full extension while standing.
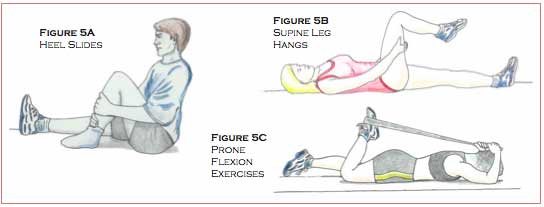
Heel slides, supine leg hangs, and prone flexion exercises with the Flexband® (Figures 5A, 5B, and 5C) can be used to restore flexion of the injured knee. Heel slides are conducted with the patient lying on the back, sliding the heel towards the buttocks until tension is felt; the position is then held for one to two minutes. Then the heel slides down into full extension. This exercise should be repeated ten times, once every waking hour. See Figure 5A.
Supine leg hangs are conducted with the patient lying on the back, grasping the hands behind the thigh and lifting the thigh towards the chest with the leg flexed. The patient then allows the leg to drop down into flexion, holding this position for two minutes. The knee is then returned to a relaxed extended position and repeated multiple times throughout the day. See Figure 5B.
Prone (on the stomach) flexion exercises can be conducted with the Flexband®. Starting out on the back, the patient creates a toe-loop with the Flexband® around the injured knee’s foot and then turns onto the stomach. The band is then swung over the head, slowly increasing the band’s tension, hand over hand, while the ankle is aligned to the buttocks. The stretch should be held for three to four minutes, repeated several times throughout the day. See Figure 5C.
Rehabilitation of the Knee: Restoring Static Restraints, Dynamic Restraints, Proprioception and Sport-Specific Skills
The static restraints of the knee are the ligaments and bony architecture that limit movement. Surgical reconstruction of the ACL restores the check-rein function of the ligament by preventing excessive forward movement of the tibia on the femur.
The dynamic restraints of the knee are the muscles and tendons that surround the knee. These muscles and tendons maintain joint position and react to changing loads and forces. Post-surgery rehabilitation depends on restoring the function of these dynamic restraints, with the main focus on restoring flexibility and strength to the hamstring and quadriceps musculature. During the initial phases of rehabilitation, isometric strength training exercises are implemented, where the muscle neither shortens nor elongates, but force is generated. A straight leg raise is an example of an isometric strength training exercise for the quadriceps musculature. Later in the post-operative rehabilitation phase, exercises will be conducted to develop eccentric strength (whereby the muscle elongates to decelerate a particular movement) and concentric strength (whereby the muscle shortens to promote a particular movement). An example of an eccentric exercise would be step-downs off of a two-inch box with the good leg. During a step-down the quadriceps of the injured leg will eccentrically fire to decelerate and control leg flexion; simultaneously the gluteus musculature of the injured leg would fire to stabilize the pelvis so the body doesn’t tilt to the side of the uninjured leg that is stepping down. An example of a concentric strengthening exercise would be forward stepups, whereby the quadriceps would concentrically contract to force the leg to extend. Rehabilitation of the dynamic restraints will aid in taking stress off of the repaired ACL, preventing re-injury.
Proprioception is best defined as reception of sensory input from mechanoreceptors (specialized cells located in the skin, muscles, tendons, ligaments, and joints), the visual field, and the vestibular system. This sensory input is processed at the spinal cord, then at the mid-brain or the more complex cerebral region. Then a reflex or motor response is generated and then regulated until the desired movement is attained. There are three main types of reflexes, the fastest being the involuntary knee jerk reflex that involves no brain processing or thought. The second fastest reflex involves thought processing through the midbrain, and the slowest reflex involves more involved thought processing in the cerebrum. Repetitive balance and movement drills can transfer reflexes that initially involve complex sensory processing in the cerebrum to the mid-brain, leading to faster more precise movement patterns. Proprioception training involves retraining and fine tuning reflexes and movement patterns through balance drills, agility drills, plyometric jumping drills, and sportspecific training. Proprioception training will increase the state of readiness of the knee joint, decreasing the chance of re-injuring the ACL upon return to sport.
Full functional rehabilitation of the knee depends on restoring static stability, dynamic stability, and proprioception. The rehabilitation program should be individualized in regards to the patient’s coordination, desire, and specific sport.
Weeks 0-2
The goals of the first two weeks of post-operational rehabilitation are to reduce swelling, restore full range of motion in extension and flexion, ambulate without the use of crutches, and sit down and stand from a seated position. Straight leg raises, side raises/abduction exercises, and assisted leg extensions to full extension (with the help of the therapist or the opposite foot) are good exercises to initiate muscle firing of the quadriceps and gluteus musculature.
Muscles located in and above the back of the thigh, the hamstrings and gluteus structures, stabilize the pelvis during ambulation and squatting-type movements. Two exercises that are instrumental in returning coordinated strength to the leg are isometric co-contractions of the hamstring and quadriceps musculature, and the other is properly performed quarter squats and full chair squats. The co-contractions should initially be conducted at 30 degrees of flexion, progressing at ten-degree intervals up to 90 degrees. Squats should be conducted at the patient’s tolerable range of motion in a controlled manner. During the squat, the patient should focus on squeezing the hamstrings and gluteus musculature during the downward movement of the squat and keep a vertical shin angle; these two actions will prevent the patient from leaning forward and placing undue stress on the knee joint. As the patient squats down, the quadriceps musculature fires to decelerate flexion of the leg, while the hamstring and gluteus musculature fire to decelerate the pelvis from rotating forward. The hamstring musculature also aids the reconstructed ACL in its check-rein function on the tibia. These exercises are crucial in developing the coordinated muscular activity of the hamstring, gluteus and quadriceps musculature that is necessary for a normal walking gait during full weight-bearing on a flat surface, as well as walking up and down stairs and getting into a seated position.
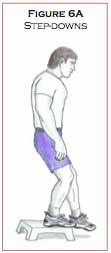
Step-downs (Figure 6A) are another useful exercise that can be included in the second week of post-operational rehabilitation. For this exercise, the patient stands with both legs on a designated raised surface and then steps down to the ground with the non-injured leg. These exercises should be conducted in front of a mirror to ensure proper technique. Apprehension in flexing the injured leg or weakness in the gluteus musculature on the same side will cause the patient’s pelvis to drop down to the side of the leg that is stepping down. Correct technique of step-downs is necessary for the patient to maintain hip stabilization, prevent pelvis drop, and proper cocontraction of the hamstring and quadriceps musculature of the injured leg to achieve a controlled leg flexion as the other foot touches the ground surface. Step-downs should commence at two inches off the ground for 25 controlled repetitions. The step-down height can be increased to four, six, and eventually eight inches as the patient regains motor control of the hip stabilizers, gluteus and hamstring musculature, as well as the decelerator of leg flexion, the quadriceps musculature.
 According to Bill Knowles, director of iSPORT at the Vermont Orthopaedic Clinic in Rutland, Vermont, after ACL repair, the sutures are usually removed between ten days and two weeks post surgery. Once the wound is healed, pool therapy can begin. Bill Knowles recommends specialized pool routines for “total body training with an emphasis on hip and knee flexion and extension movements, as well as core strength exercises to include all of the muscles involved in stabilizing the torso from the hips to the shoulder.” The patient holds floatation bars while conducting various movements in the pool to improve the coordinated strength of the hip stabilizers, knee extensors and flexors, as well as the core strength musculature.
According to Bill Knowles, director of iSPORT at the Vermont Orthopaedic Clinic in Rutland, Vermont, after ACL repair, the sutures are usually removed between ten days and two weeks post surgery. Once the wound is healed, pool therapy can begin. Bill Knowles recommends specialized pool routines for “total body training with an emphasis on hip and knee flexion and extension movements, as well as core strength exercises to include all of the muscles involved in stabilizing the torso from the hips to the shoulder.” The patient holds floatation bars while conducting various movements in the pool to improve the coordinated strength of the hip stabilizers, knee extensors and flexors, as well as the core strength musculature.
After 115 degrees of leg flexion is attained, stationary cycling can commence to increase range of motion of the knee joint, as well as provide light endurance exercise. Other exercises that be used to increase range of motion and muscle coordination are swimming and the elliptical machine.
All of the above exercises included in the second week of the post-operative rehabilitation phase should be conducted to the patient’s tolerance and in a controlled setting. If swelling occurs or if there is decreased range of motion in the knee joint, the progression of the rehabilitation phase should be slowed down, the range of motion restored, and the swelling reduced.
Weeks 3-5
 In weeks 3-5, functional exercises can be added to the rehabilitation routine. The following exercises are recommended:
In weeks 3-5, functional exercises can be added to the rehabilitation routine. The following exercises are recommended:
- Balance star drills on a flat surface – balance while reaching forward with the good leg or opposite arm.
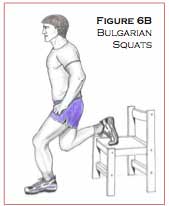
- Bulgarian squats – with the good leg up on a bench/chair, perform the squat with the injured leg (Figure 6B).
- Pelvic bridge lying on the back, legs flexed to 90 degrees, lift the buttocks off of the floor while squeezing the glutes and the hamstrings.
- Balance drills on a disco-sit/curved seat cushion.
- Ball squats without weights, and later with weights held by the patient during the squat (Figure 6C).
- Single leg Romanian deadlifts – on a step box, bend forward from the trunk while holding a weighted ball with both hands in front, and balance on the deconditioned leg (Figure 6D).
- Leg Presses – single leg.
- Abduction, adduction, single leg extensions, calf raises.
- Ball tosses while balancing on a balance board.
- Lunges.
- Exercise ball hamsting curls.
- Towel stretches and standing extension stretches with resistive tubing.
Delayed onset muscle soreness is expected. If there is normal range of motion, no immediate swelling, and muscle pain dissipates in two to three days, the patient can continue to progress with the rehabilitation routine. 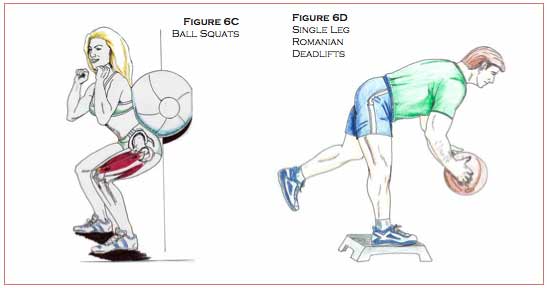
Weeks 6-8
- Progress to heavier weights with the above exercises.
- Continue towel stretches and Flexband® stretches to maintain and increase range of motion of the knee in both flexion and extension.
- Proprioception drills, e.g. wobble board exercises balancing on two legs, balancing on one leg, ball tosses while balancing, done with the eyes closed for advanced drills.
Weeks 8-11
Romanian deadlifts.
Light sport-specific training, e.g. a basketball player shooting free throws or conducting passing drills.
Week 12
If the patient has full range of motion and strength of the musculature surrounding the knee, he or she may start a running program: Treadmill running for ten to 15 minutes, level surface running on cement for 2030 minutes, hill running, sprinting, figure 8’s, side sliding, start and stop shuttle runs, and 45-degree cutting. Jumping drills can teach the athlete how to land softly while sitting back and incorporating the hamstring and gluteus musculature. These agility drills can be progressed as tolerated.
4-6 Months
The patient can return to full light sport participation if assuming full range of motion, 90 percent strength of the hamstrings and quadriceps musculature (as compared to the healthy leg) and success in conducting all of the agility drills with no pain or swelling.
The therapist should explain to the patient that while it is okay to return to full light sport specific training, it can take up to three months of participation in their sport to regain the complex movement patterns of the particular sport. It may take up to seven months to a year for “ligamentization” of the grafted tissue, whereby the grafted tissue becomes almost identical, in its properties, to the original anterior cruciate ligament.
Post Surgical Treatment of the Anterior Cruciate Ligament at Dr. Dubin’s office
Treatment of the repaired ACL at this office would commence after the sutures are removed and the wound is healed, approximately two weeks post-surgery. Treatment would consist of:
- Specific muscle work, including active release technique, to free up soft tissue motion of the surrounding knee musculature, helping to restore normal range of motion of the knee in flexion and extension;
- Ultrasound and electric muscle stimulation combo therapy to break up scar tissue and restore normal muscle tone;
- Patella mobilization techniques.
The above treatment protocols would aid in breaking up scar tissue and restoring proper joint and soft tissue range of motion.
Good communication and repeat follow-ups among the physician and therapists are crucial in creating and maintaining the optimum treatment protocol for pre- and postsurgery rehabilitation of the anterior cruciate ligament, allowing for a safer and quicker return of the athlete to their particular sport.
Acknowledgements
This paper was made possible with the help and expertise of Keith Callanan MPT, CSCS, of Elite Physical Therapy (781-297-0979) and Bill Knowles ATC, CSCS, Director of iSPORT (802-422-6191). I recommend their services to all patients who are suffering from anterior cruciate ligament injuries.
If you have any questions or want to set up an appointment with Dr. Dubin please call 617-471-2444.
References
1) Shelbourne DK, Rowdon GA: Anterior Cruciate Ligament Injury. The Complete Athlete, Sports Med 17(2) 132-140, 1994.
2) Rodeo SA, Arnoczky SP, Torzilli PA, Hidaka C, Warren R: Tendon-healing in a bone tunnel. J Bone Joint Surg 75A: 1795-1803, 1993.
3) O’Neill, Daniel F. , New Hampshire Knee Center, The 1st Week Post-Op 2003
4) Rinsberg MA, Mork M, Jenssen HK, Holm I: Design and Implementation of a Neuromuscular Training Program Following Anterior Cruciate Ligament Reconstruction. J of Othopaedic and Sports Physical Therapy 2001; 31 (11): 620-631.
5) Hewett TE, Paterno MV, Myer GD: Strategies for Enhancing Proprioception and Neuromuscular Control of the Knee. Clinical Orthopaedics and Related Research 2002; number 402: 76-94.
6) Bill Knowles ATC, CSCS, director of iSPORT at the Vermont Orthopaedic Clinic, Rutland, Vt.
7) Keith Callanan, MPT. Owner of Elite Sports. Inc. Stoughton, Ma.
8) Amiel D, Kleiner JB, Roux RD, Harwood FL, Akeson WH: The Phenomenon of “Ligamentization”: Anterior Cruciate Ligament Reconstuction with Autogenous Patellar Tendon. J of Orthopaedic Research 1986; (4): 162-172.
Additional references
Reid D: Sport Injury Assessment and Rehabilitation. 1992.
Norman, SW: The Knee. 1994.

